TAILBONE PAIN (also called Coccyx pain, Coccydynia, or Coccygodynia) ![]()
In order to help patients with tailbone pain, and their treating physicians, Dr. Foye has written a brief summary, below. This summary outlines some common causes, symptoms and treatments for tailbone pain. As with any medical condition, it is recommended that patients seek care from a physician who is knowledgeable and experienced in treating other patients with the same condition or similar diagnoses. Unfortunately, some patients report difficulty finding physicians with expertise at evaluating or treating tailbone pain. Hopefully, the information below will provide some basic education for patients, their families, and their caregivers.
COCCYDYNIA DEFINITION:
Coccydynia is the medical term for pain of the coccyx (tailbone). Coccydynia is also known as coccygodynia. Patients will often simply refer to this as “tailbone pain” or “coccyx pain“.
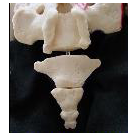
The coccyx, or tailbone, is a group of small bones. These bones are the lowest part of the human spine. They are located at the back of the pelvis, between the buttocks, above the anus.
CAUSES OF TAILBONE PAIN:
Pain of the coccyx (coccydynia) can be due to a variety of causes:
Direct trauma to the coccyx can result in coccyx fractures, dislocations, alignment abnormalities, etc.. Examples of trauma to the coccyx could include a fall onto the tailbone, pregnancy (and especially childbirth, which can put substantial pressure onto the coccyx as the baby moves down within the pelvis), prolonged sitting (especially sitting on a hard surface, or sitting on a narrow surface such as a bicycle seat, or increased sitting due to immobility because of an injury at a totally unrelated body region).
Pain referred to the coccyx from nearby body regions: Sometimes pain can be referred to the coccyx from medical conditions at adjacent body regions. Thus, it is often worthwhile to consider whether any medical conditions within the pelvis and rectum may actually be the underlying source of the pain that the patient feels predominantly at the coccyx. Other conditions that present with pain in the buttock region can include bursitis (inflammation of a bursa, which is a fluid-filled sac, of which there are many throughout the body).
“Idiopathic” coccyx pain: In many cases, the exact cause of the coccydynia remains unknown. In these cases, the patient may not have any history of trauma to the region, nor any associated medical conditions in the pelvis or rectum.
SYMPTOMS:
Certainly the classic, defining symptom for coccydynia is exquisite, focal pain at the coccyx. The pain from the coccyx may travel (radiate) down into the floor of the pelvis (e.g., into the lower genital region). Coccydynia is frequently exacerbated by sitting, and especially by prolonged sitting or sitting on a hard surface. Initial movement into the standing position (after sitting) may also be painful. Most patients are able to locate their own coccyx bones, and will indicate this spot as the primary focus of their pain. Patients will recognize the coccyx location as being in the midline between the gluteal muscles (buttocks). A patient wearing a belt would generally find their coccyx to be perhaps 4 to 7 inches below where the belt-line crosses the middle of their lower back. The coccyx is located just slightly above the anus, and sometimes coccyx pain can be exacerbated by defecation, especially if the bowel movement is particularly large or hard. Unfortunately, coccydynia can be severe and persistent, and can substantially decrease the quality of life for the affected patient.
MAKING THE DIAGNOSIS:
Usually, an experienced physician can make the diagnosis of coccydynia based upon a careful history and physical examination. Additional diagnostic tests can include x-rays and other imaging studies. Consultations with other physicians may be helpful if it is felt that the coccyx pain is originating from medical conditions of the gastrointestinal tract (e.g., the rectum), or originating from medical conditions of the reproductive organs (uterus, ovaries, etc.).
TREATMENT:
There are a wide variety of treatments available for coccyx pain. Often, a combination of treatment approaches is necessary in order to give adequate relief.
Avoiding exacerbating factors: Patients can avoid exacerbating factors by minimizing prolonged sitting and by avoiding sitting on hard surfaces.
Cushions: Sitting on cushions can be helpful, and especially sitting on “donut” cushions (which have a hole cut out in the center, where the coccyx would otherwise be pressing) or “wedge” cushions (which have a wedge-shaped triangle cut out in the rear of the cushion, where the coccyx would otherwise be pressing).
Medications taken by mouth: Pain may be decreased by the use of a variety of medications taken orally. These include anti-inflammatory medications (such as ibuprofen, etc.), opioid/narcotic analgesics (such as Percocet, etc.), medications used to treat nerve pain, and a variety of other medications.
Medications given by local injection: In patients who are not receiving adequate relief via cushions and oral medications, medications given by local injection may provide substantial relief and may provide complete resolution of the pain. Unlike caudal (epidural) steroid injections, nerve blocks for coccydynia may focus on using a local anesthetic to block (temporarily shut-off) the nerves that carry painful signals from the coccyx. These injections may especially target the ganglion Impar, which is part of the sympathetic nervous system. Dr. Foye very strongly recommends the use of fluoroscopic guidance (which is similar to x-ray images viewed live on a video monitor during the procedure) for any such injections, in order to most accurately place the injection and thus minimize the patient’s risks and maximize the patient’s benefits. If the initial injection does not provide enough relief, then it may be repeated to achieve further benefit for the patient.
Coccyx surgery: Various surgeries of the coccyx have been considered somewhat controversial, and may carry significant risks. Coccyx surgery would generally only be considered in patients who have severe, persistent coccyx pain despite non-surgical treatments, including the use of oral medications and focal injections performed under the guidance of fluoroscopy. There are a small percentage of patients with tailbone pain who may require surgical removal of the coccyx (coccygectomy). Fortunately, most patients respond well enough to non-surgical treatments (especially including the injections) that they no longer need to consider undergoing surgical treatment.