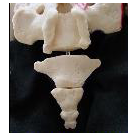
- At the time of surgery to remove the coccyx (coccygectomy), it is somewhat variable what the surgeon does.
- Sometimes the tailbone is partially removed, sometimes completely removed.
- Surgeons differ in their opinions as to how important it is or isn’t to try to re-attach the pelvic floor tendons that were previously attached to the coccyx.
- After surgery, most people do not have problems due to losing the natural attachments to the coccyx.
- But perhaps 5% or less may develop a complication called pelvic floor prolapse, where the floor of the pelvis starts to sag downward, which can cause problems with bowel and bladder function.
Regarding complications and side-effects from coccygectomy (surgical removal of the tailbone), please click on the links below:
To come to Dr. Foye’s Tailbone Pain Center:
Tailbone Pain Book:
To get your copy of Dr. Foye’s book, “Tailbone Pain Relief Now!” click on this link: www.TailbonePainBook.com
 Book: “Tailbone Pain Relief Now! Causes and Treatments for Your Sore or Injured Coccyx” by Patrick Foye, M.D.
When there is skin breakdown of ulceration of the skin over the coccyx, it is worth looking for a cause.
- Sometimes people develop a bed-sore of the skin behind the sacrum and coccyx after spending too much time laying in bed. (The medical term for a bedsore is a “decubitus ulcer”.)
- Usually, a bedsore will heal once the person is more active (spending less time laying in bed) or with more frequent repositioning in bed (such as having the nurses or family roll the patient in bed every two hours, in order to give the skin a chance to heal and ‘breathe’).
- But in some cases the skin breakdown may persist or it may come back.
- Or sometimes the skin has delayed healing after a coccygectomy (surgical amputation of the coccyx). Normally a surgical site will close and heal, but sometimes this is delayed or there are problems with healing at the post-operative site. There may even be “dehiscence”, which is also called “wound separation.” (Dehiscence means that the edges of the wound no longer meet, and this can result in delayed healing and increased risk for the wound to become infected.)
If the skin breakdown persists or returns, consider these possible causes:
1) Infection? I would think that the first step would be trying to differentiate whether the lack of forward healing seems to be caused by an underlying infection or not. Typical signs of infection include fever, chills, redness/warmth of the skin in the area, blood work showing increased white blood cells (wbc’s), blood work showing increased ESR (erythrocyte sedimentation rate) or CRP (ESR and CRP are both general signs of inflammation, which can include infection), imaging findings of inflammation on MRI (including specifically looking to see whether any such inflammation is located within the substance of the bone [bone infection is called osteomyelitis] or whether any such inflammation is located in the soft tissue structures outside of the bone [including skin infection, which is called cellulitis]).
2) Underlying immune compromise? Particularly if there is any recurring infection, then it would be worthwhile asking your primary care doctor to check whether there is any underlying compromise of your immune system that might be putting you at risk for these persistent or recurrent infections. This would typically mean checking for things like HIV/AIDS, certain cancers especially certain leukemias (blood cancers involving the white blood cells), etc.. A consultation with an “Infectious Disease” (ID) physician specialist may be helpful.
3) Nutritional deficiencies? Admittedly, most people eating a normal diet probably do not have a nutritional deficiency that is responsible for a wound failing to heal. But it is worth considering, especially if someone is only eating some kind of very restricted diet that fails to give a balance of multiple food groups.
4) Anal fistula or rectal fistula? Sometimes people develop a small tear inside the anus or within the wall of the rectum. Eventually this can form into a tunnel or track (“fistula”). This tunnel can take stool or bacteria from the bowels into nearby tissue, causing infection of those tissues. To evaluate for this possibility typically would require seeing a gastroenterologist (a physician who is a “G.I.” [gastrointestinal] specialist). Tests for this sometimes could involve putting contrast (medical dye) into the rectum and seeing if it fills up the tunnel, which would then be visible on imaging studies done after the dye is put in place.
Treatments can vary
- Antibiotics can be given to resolve infection at the wound site.
- IV antibiotics: If the infection is located within the bone, then typically get about X. would need to be several weeks of intravenous antibiotics.
- Debridement: The physician or surgeon may need to remove some of the infected tissue. This essentially removes the bulk of the infection (bacteria).
- Coccygectomy? If there a substantial possibility that there is infection within the substance of the coccyx bones themselves (osteomyelitis = bone infection), then in addition to several weeks of intravenous antibiotics (which usually should do the job) one potential consideration would be whether to surgically remove the tailbone as a means of removing the infected bones. This would have some risks, since even without an infection being present before surgery, surgical removal of the coccyx (coccygectomy) is associated with a relatively high rate of infection during the initial weeks or months after the surgery. Presumably, cutting through infected bone would be associated with an even higher rate of infection than cases where the surgeon is cutting through bone that is NOT infected. Still, removing the infected bone would essentially be removing the bulk of the infected tissue, and even if there was some persistent infection within the soft tissue structures after the surgery, those types of soft tissue infections do tend to respond antibiotics (soft tissue infections respond much better and quicker to antibiotic treatment, as compared with bone infections).
Regarding complications and side-effects from coccygectomy (surgical removal of the tailbone), please click on the links below:
To come to Dr. Foye’s Tailbone Pain Center:
Tailbone Pain Book:
To get your copy of Dr. Foye’s book, “Tailbone Pain Relief Now!” click on this link: www.TailbonePainBook.com
 Book: “Tailbone Pain Relief Now! Causes and Treatments for Your Sore or Injured Coccyx” by Patrick Foye, M.D.
MRI studies of the tailbone show lots of details of the anatomy of the coccyx region.
But the doctor needs to know which images to look at for the different types of details that can be seen.
- T-1 images are best for looking at bony structures like the actual bones of the tailbone (coccyx).
- T-2 images are not as good as T-1 images at showing details of the bones.
- But T2 images are better than T1 images at detecting inflammation.
- Inflammation is important to look for, since this can be a sign of joint arthritis, joint dislocations, bone fractures, bone infections, and other abnormalities.
- “STIR” images also show inflammation (similar to T2 images).
To come to Dr. Foye’s Tailbone Pain Center:
Tailbone Pain Book:
To get your copy of Dr. Foye’s book, “Tailbone Pain Relief Now!” click on this link: www.TailbonePainBook.com
 Book: “Tailbone Pain Relief Now! Causes and Treatments for Your Sore or Injured Coccyx” by Patrick Foye, M.D.
After coccygectomy (surgical removal of the tailbone) as a treatment for tailbone pain (coccyx pain), should patients worry about whether sex will be painful?
- I don’t know any published research on this one way or the other, but for patients I have treated after they have had coccygectomy, I don’t recall many that have reported problems with sex after the surgery.
- It’s possible, though, that people are embarrassed to mention it or I am not asking in a way that gets the best info..
- In general, people in pain may have less interest in sex or may fear that the physical nature of sex may worsen their pain, especially pain in the pelvic area, which includes the tailbone (coccyx).
- So, anything that helps to decrease someone’s pain (whether the treatment is medications, injections, or surgery) may subsequently helped to improve their interest in sex and their ability to comfortably engage in sex.
Body position during sex: how much pressure on the tailbone?
- The specific position that the person is in during sex may also be important.
- In general, positions that put direct pressure (such as your body weight, or another person’s body weight) onto the tailbone are more likely to be painful.
- So, a person laying on their back would be more likely to have tailbone pain if they are slightly reclined, as compared with someone laying flat. (While laying flat, most of the body weight is on to the sacrum, rather than the coccyx).
- People with tailbone pain may need to work together with their partners to find the positions that are least likely to cause worsening of the tailbone pain. Examples include figuring out who should be ‘on top’.
Vaginal versus anal sex
- Also, it is important to distinguish between vaginal intercourse versus anal intercourse.
- My guess is that anal sex would potentially be much more problematic for people with tailbone pain, whether they had surgery for the coccyx or not. But again I don’t have actual research/surveys to support that, just my expectation based on the anatomy there.
To come to Dr. Foye’s Tailbone Pain Center:
Tailbone Pain Book:
To get your copy of Dr. Foye’s book, “Tailbone Pain Relief Now!” click on this link: www.TailbonePainBook.com
 Book: “Tailbone Pain Relief Now! Causes and Treatments for Your Sore or Injured Coccyx” by Patrick Foye, M.D.
- The best and worst of sitting surfaces varies from person to person with tailbone pain.
- Many people find a hard surface to be better because then they can sit on the other to sit bones (the ischial bones, or ischial tuberosities, which is the bony spot at the bottom of each buttock cheek), and avoid or minimize having the seat make contact with the coccyx.
- If the seat is too soft, then the ischial bones just sink into the cushion which lowers the coccyx to a point where it makes contact with the seat/cushion.
- Other people with tailbone pain prefer a softer surface.
- If the chair or cushion is too hard, then pressure from the chair or cushion may cause excessive pressure on other nearby body regions, such as the ischial bones (the “sit bones” at the bottom of each buttock cheek), or on the piriformis muscle is the lower part of each buttock.
- Sometimes the sciatic nerve in the area of the piriformis muscle can also be affected, causing nerve pain that shoots down the leg.
To come to Dr. Foye’s Tailbone Pain Center:
Tailbone Pain Book:
To get your copy of Dr. Foye’s book, “Tailbone Pain Relief Now!” click on this link: www.TailbonePainBook.com
 Book: “Tailbone Pain Relief Now! Causes and Treatments for Your Sore or Injured Coccyx” by Patrick Foye, M.D.
A tailbone fracture (“a broken coccyx”) takes longer to heal than fractures at most other body regions.
There are multiple reasons for this:
- Unlike fractures at many other body regions, there is no cast, splint, or brace that can be put on a fractured tailbone.
- Alike fractures at many other body regions, there is no way to avoid putting your body weight on the fracture (unless you totally avoid sitting for several weeks).
- So, a tailbone fracture never really gets a chance to rest and recover the way that fractures at most other body regions do.
- So, it is not surprising that much longer than fractures that most other body regions.
- It’s also not surprising that tailbone fractures are more likely to go on to develop chronic, ongoing pain.
To come to Dr. Foye’s Tailbone Pain Center:
Tailbone Pain Book:
To get your copy of Dr. Foye’s book, “Tailbone Pain Relief Now!” click on this link: www.TailbonePainBook.com
 Book: “Tailbone Pain Relief Now! Causes and Treatments for Your Sore or Injured Coccyx” by Patrick Foye, M.D.
Some patients ask whether medical marijuana can be used to decreased tailbone pain (Coccyx pain, coccydynia).
Is marijuana legal in your state? Can you use it for tailbone pain?
- Whether or not marijuana is considered legal depends on the state and/or country that you live in.
- Overall, compared with the last 60 years or so, the tide has turned. There are an increasing (dare I say “growing”) number of states are allowing for more liberal use of medical marijuana and even recreational marijuana.
- It depends on the state you live in.
- Some states classify marijuana as illegal regardless of whether it is for medical use or for recreational use.
- Some states considered medical marijuana to be legal, but recreational marijuana to be illegal.
- Some states consider marijuana to be legal regardless of whether it is for medical use or for recreational use.
- Of those that only allow marijuana for medical use, some states are more strict than others on which particular medical conditions the marijuana can be prescribed for.
- Here in New Jersey, medical marijuana is very restricted. In New Jersey, medical marijuana can only be prescribed to certain specific conditions (ALS, multiple sclerosis, etc.). Coccyx pain (tailbone pain) is NOT among those conditions for which marijuana can be legally prescribed in New Jersey. In New Jersey, the law also limits it so that prescription of medical marijuana can only be done by specially-designated physicians (the vast majority of physicians in NJ can not prescribe it).
- Interestingly, at the federal level my role on a currently remains illegal. Most likely that will eventually change, since it is problematic to send mixed messages where the federal government says something is illegal in the entire country but the individual states that make up the country say that it is legal within their own state.
To come to Dr. Foye’s Tailbone Pain Center:
Tailbone Pain Book:
To get your copy of Dr. Foye’s book, “Tailbone Pain Relief Now!” click on this link: www.TailbonePainBook.com
 Book: “Tailbone Pain Relief Now! Causes and Treatments for Your Sore or Injured Coccyx” by Patrick Foye, M.D.
For people with Tailbone Pain, the x-rays/MRI/CT-scans often FAIL to even include the Tailbone, even though that is the source of the person’s pain
- Many patients experience frustration with finding out that their local radiologists/doctors did not even include the tailbone in their imaging studies.
- As crazy as that is, unfortunately I see this essentially every week in my new patients, regardless of what state or country they come from.
- People suffer for months and years while being told their imaging studies were normal, only to eventually find out that the imaging studies never actually included the tailbone (even in cases where the patient explicitly told the ordering physician and the radiology technician that the tailbone was the source of pain).
- This is one of the reasons why I have my new/incoming patients gather up their previous radiology reports and previous radiology imaging studies (usually on a computer CD, or sometimes on the more old-fashioned films). That way the patient and I can look through the images and radiology reports to determine whether they even included the tailbone at all.
- Also, in the vast majority of new/incoming patients, I typically get sitting-versus-standing x-rays of the coccyx/tailbone done, since this specifically includes looking for unstable joints at the tailbone (coccygeal dynamic instability) which can really only be detected on x-rays that are done while sitting (which very few radiology centers have ever heard of).
To come to Dr. Foye’s Tailbone Pain Center:
Tailbone Pain Book:
To get your copy of Dr. Foye’s book, “Tailbone Pain Relief Now!” click on this link: www.TailbonePainBook.com
 Book: “Tailbone Pain Relief Now! Causes and Treatments for Your Sore or Injured Coccyx” by Patrick Foye, M.D.
- For people who have the worst pain while they are making the transition from sitting to standing, this is often due to unstable joints at the tailbone (coccygeal dynamic instability).
- Basically, a fall or other trauma can injure the ligaments that would normally hold the individual bones of the coccyx in a normal and stable alignment.
- When those ligaments are no longer functioning properly (due to sudden, traumatic injury, or sometimes even just from gradual loosening over the years), one or more of the joints of the tailbone can become unstable.
- Sitting puts body weight/pressure on the joints, often causing a partial dislocation.
- When someone stands up suddenly, the body weight/pressure is removed and the tailbone may “snap” back into a more normal alignment.
- That transition/snap is often VERY painful for patients.
- After those few moments of worsened pain during the transition from sitting-to-standing, many patients find that their pain is better for a while (while they are standing or walking), only to return again the next time they sit down.
- Unstable joints of the tailbone can only be diagnosed by having x-rays done while you are sitting and then comparing those images with the position of your coccyx while you are standing.
- Unfortunately, very few radiology centers perform coccyx x-rays while you are sitting. This causes many patients to suffer in pain while the cause remains unrecognized.
To come to Dr. Foye’s Tailbone Pain Center:
Tailbone Pain Book:
To get your copy of Dr. Foye’s book, “Tailbone Pain Relief Now!” click on this link: www.TailbonePainBook.com
 Book: “Tailbone Pain Relief Now! Causes and Treatments for Your Sore or Injured Coccyx” by Patrick Foye, M.D.
Just this week, our medical article was published on the topic of a chiropractic actuator (also called an actuator gun or activator gun) being used to apply force to the coccyx (tailbone), resulting in new-onset tailbone pain.

ABSTRACT:
- Coccyx pain (also called coccydynia, or tailbone pain) has a broad range of etiologies, including traumatic and non-traumatic causes.
- Iatrogenic etiologies of coccydynia are rarely reported.
- This is the first report of iatrogenic coccydynia due to the use of a chiropractic actuator.
- An actuator (also known as an activator adjusting instrument, actuator gun or activator gun) is a spring-loaded hand-held device that delivers a sudden mechanical force to the anatomic site where it is applied.
- We report a patient whose neck and shoulder pain were assumed to be due to cranio-dural stress syndrome.
- An actuator was used to deliver forces to the coccyx region in hopes that relieving dural tension at the coccyx might improve her neck pain, which it did not.
- Upon receiving the actuator treatments to her coccyx, she had immediate onset of coccyx pain, which lasted for many months.
- The patient had no prior history of coccyx symptoms or trauma.
- She eventually presented for treatment at our Coccyx Pain Center, on an academic medical school campus.
- Actuator use at the coccyx should be added to the list of causes of tailbone pain.
- Patients and clinicians should be aware of this risk.
The full article is available for free online here:
http://www.webmedcentral.com/wmcpdf/Article_WMC004998.pdf
To come to Dr. Foye’s Tailbone Pain Center:
Tailbone Pain Book:
To get your copy of Dr. Foye’s book, “Tailbone Pain Relief Now!” click on this link: www.TailbonePainBook.com
 Book: “Tailbone Pain Relief Now! Causes and Treatments for Your Sore or Injured Coccyx” by Patrick Foye, M.D.
|
Book Now Available! Click on the book to get it now:
|